By now we are all aware that we are in the midst of a “global public health emergency” due to a novel coronavirus known as SARS-CoV-2, which causes the disease COVID-19. The “novelty” of this virus only refers to the fact that it is new; this is not a romantic title for a deadly virus. In all seriousness, the virus that arose late last year in Wuhan, China has now spread to over 25 other countries and has killed, on average, at least 2.3% of the > 90,000 people it has infected (fatality rate increases in older populations; 8 to 14.8 %). As a result scientists and doctors are racing to catch pace with the virus, not only to develop a vaccine, but to characterize how this coronavirus behaves in its victims.

Recently, the media has caught wind of some of the reports coming out of the laboratories and clinics, and in what appears to be a hast of misunderstanding have produce more fear and misinformation. The news media has reported that some people who had COVID-19 were re-infected with SARS-CoV-2 after recovering and being discharged from the hospital. Given that there is no precise treatment or approved vaccine, the idea that one could contract the virus again, after just having it, portends that SAR-CoV-2 is insidious; and has sent many people into a panic as its characterizes the virus as being monsterous and unstoppable. It would also mean that SARS-Cov-2 is operating beyond the conventions of virology and immunology.
However, that is not the case and here is why:
SARS-CoV-2 Similar to SARS & MERS
SARS-CoV-2 (Severe Acute Respiratory Syndrome Coronavirus 2) previously known as 2019-nCOV is the third pathogenic coronavirus to cause severe respiratory disease and death in humans; following after SARS-CoV and MERS-CoV ( Middle-East respiratory syndrome coronavirus). All three viruses are in the family Coronaviridae, belonging to the subgroup sarbecvirus. SARS-CoV-2 is a zoonotic virus, meaning it has crossed over from infecting animals to humans. These three human coronaviruses originated in bats, but each evolved in different intermediate mammals before crossing to humans. While the first SARS-CoV virus moved from bats to civets, and MERS-CoV from bats to camels, SARS-CoV-2 is suspected of jumping from bats to pangolins before entering humans (research is still being conducted to confirm the intermediary species for SARS-CoV-2).

SARS-CoV-2 is likely to behave similarly in virology to its predecessors. SARS-CoV-2‘s genome is made-up of single stranded RNA (about 30 nucleotides long), which encodes for 4 major proteins that make up its structure: spike protein ( a type I glycoprotein), membrane protein, envelope protein, and nucleocapsid protein. This means that structurally, the RNA strand is encapsulated and enveloped by a membrane with protein spikes protruding outwards to the surface. These glycoprotein spikes allow entry into cells by binding with angiotensin-converting enzyme 2 (ACE2) in a complex process involving virus-cell fusion. ACE2 is widely found on multiples organs and tissues in the body, and responsible for regulating heart & kidney function thereby controlling blood pressure. It has been determined that SARS-CoV-2 and SARS-CoV share 80% of their genome and bind with similar affinity to human ACE2. MERS-CoV uses its spikes to gain entry into human cells also, but unlike SARS-CoV and SARS-CoV-2 its entry receptor is dipeptidyl-peptidase 4.
Though similar in nature, SARS-CoV-2 has a relatively higher transmissibility, resulting in its rapid spread.
False Negative, Not Reinfection
As for whether individuals can be reinfected by SARS-CoV-2 immediately after recovering, the likelihood of that is slim. Consider a recent case-report from China, published in the International Journal of Infectious Diseases, in which a 46 year old woman was admitted to the hospital and, diagnosed and treated for COVID-19 after presenting with fever, sore-throat, cough, and respiratory distress. Swab test of her mouth and throat were positive for SARS-CoV-2. The patient was tested repeatedly over the course of treatment for SARS-CoV-2 and monitored thereafter. Guidelines from the National Health Commission in China required 2 consecutive negative tests, with an interval of 24 hours, before patients could be considered for discharge. The patient in this case received two negative tests, on the January 28th and January 30th, and had a normal body temperature, improved respiration, and scans of her lung showed lesions were disappearing. However, on February 2 she tested positive for the virus again.
Many have mistaken reports of cases like these to mean that individuals are getting reinfected with the virus after apparently recovering. However, what this means is that the tests returned a false negative result. This can occur due to several factors, such as site of specimen collection, experience of the person running the test, and the actual viral load of the specimen sample.
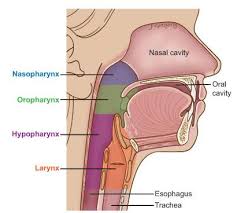
Tests are generally conducted using samples collected from swabbing the nose or the mouth of the patient. The receptor by which the virus enters the cell is more abundant in the lungs compared to the upper respiratory tract, making it more likely for the viral RNA to be found in high quantity in the lungs versus the mouth and nose. A low viral load in the specimen collected may make it difficult to detect, if the test is not sensitive enough. Meaning that the test may not detect the virus even though it is still present. Additionally, the person testing the sample may make technical errors that lead to a false negative result.
The researchers in this case specify that testing bronchoalveolar lavage fluid is more accurate in terms of detection, however this method puts clinicians at increased risk of exposure. They suggest that both nasal and oral swab tests be performed to reduce false negatives, and state that SAR-CoV-2 RNA tests be combined with other detection methods such as antibody detection or next generation sequencing to ensure validity of results.
Other Cases of Relapsed Positive Tests
In another case in China, a 54 year old man with confirmed diagnosis of COVID-19 also tested negative in two consecutive tests ( 24 hours apart) in which samples were gathered by swabbing his throat. During this time, like the 46 year old woman, he was asymptomatic. For three days he had no fever or cough and clinical signs of improved lung function. However, further testing identified he had a high viral load for SARS-CoV-2, again.
Due to numerous reports that patients, like these in China and the United States, were asymptomatic before testing positive again for SARS-CoV-2, the media has further misinterpreted this to mean that asymptomatic people are walking around unaware that the are infected and thereby infecting others. What they neglect to mention is that these were people who had already been diagnosed with COVID-19 had apparently recovered, and not people who are unaware of being sick to begin with (mild symptoms are still symptoms whether recognized as illness or not).
Summary
Once infected by a virus, whether it be SARS, MERS, or Influenza, one cannot acquire that virus again, unless it has mutated; whereby infection would be caused by a much different strain. This is because the body has developed antibodies against the virus to defend itself from future infection. That is the nature of virology and immunology.

Yes, SARS-CoV-2 is a novel ( new or previously unknown) coronavirus, the latest of a string of coronaviruses to infect humans, but it behaves similar to SARS and MERS, and is not a superbug capable of mutating so rapidly as to reinfect hosts who have recovered from COVID-19. Those who recover from COVID-19 would have antibodies against SARS-CoV-2, preventing them from being re-infected. In fact, a recent study, conducted in mice inoculated with SARS-CoV (the first SARS) blocked the entry of SARS-CoV-2 into cells, suggesting that immunity against one pathogenic coronavirus may protect against the others ( due to the 80% genomic similarity of the two SARS viruses).
SARS-CoV-2 has a relatively high rate of transmissibility compared to SARS and MERS, an thus has spread faster and infected far more people. How soon after infection does one become contagious is still being investigated. However, as the virus is currently recognized as being spread by those with COVID-19, doctors are monitoring cases of confirmed COVID-19 persons to understand viral clearance and infectivity in those who have recovered. It remains unknown whether patients who have been discharged from the hospital or who are in convalescence, but otherwise asymptomatic, remain contagious and if so for how long. For this reason 14 day quarantine after recovery is prescribed.
References
Alexandra C. Walls, Young-Jun Park, M. Alejandra Tortorici, Abigail Wall, Andrew T. McGuire, David Veesler, 2020. Structure, Function, and Antigenicity of the SARS-CoV-2 Spike Glycoprotein. Cell Vol 180 p 1-12
Dabiao Chen, Wenxiong Xu, Ziying Lei, Zhanlian Huang, Jing Liu, Zhiliang Gao, Liang Peng, 2020. Recurrence of positive SARS-CoV-2 RNA in COVID-19: A case report,
International Journal of Infectious Diseases, https://doi.org/10.1016/j.ijid.2020.03.003.
Jing-feng Zhang, Kun Yan, Hong-hua Ye, Jie Lin, Jian-jun Zheng, Ting Cai, 2020.
SARS-CoV-2 turned positive in a discharged patient with COVID-19 arouses concern regarding the present standard for discharge. International Journal of Infectious Diseases, https://doi.org/10.1016/j.ijid.2020.03.007.
Junwen Luan, Yue Lu, Xiaolu Jin, Leiliang Zhang, 2020. Spike protein recognition of mammalian ACE2 predicts the host range and an optimized ACE2 for SARS-CoV-2 infection. Biochemical and Biophysical Research Communications, https://doi.org/10.1016/j.bbrc.2020.03.047.

Hello, i read your blog occasionally and i own a similar one and i was just wondering if you get a lot of spam responses? If so how do you protect against it, any plugin or anything you can advise? I get so much lately it’s driving me mad so any support is very much appreciated.
LikeLike